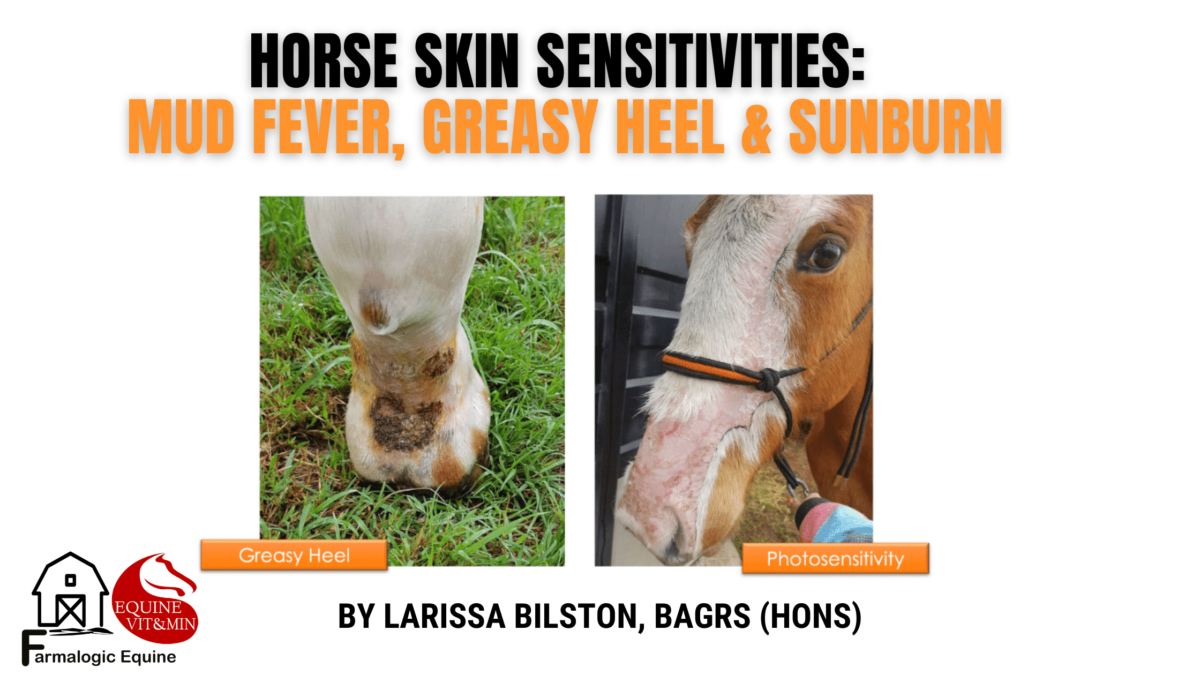
Mud fever in Summer? Sunburn in Winter?
Why would a horse not standing on muddy ground get mud fever or greasy heel? What causes severe sunburn on the nose of a pink-skinned horse on a cloudy day or in a shaded paddock? Why doesn’t the skin respond quickly to anti-bacterial creams, washes and sunscreen?
Winter Mud Fever/Greasy Heel
Greasy heel (also known as mud fever) can become a very painful and frustrating condition to manage, especially during wet weather and under humid conditions. The condition seems to affect some horses more than others, and often affects the pink skin under white socks more often than dark skin.
During very wet weather and in poorly drained yards or paddocks, horses often develop small scabs on the lower legs and heels. This initially starts with a breakdown in the skin barrier which can then let infection in. The cracked and inflamed skin develops a ‘greasy’ discharge as the broken skin becomes infected. Greasy heel can become so painful it causes lameness.
Treatment involves removing horses from wet ground, keeping the affected areas dry and treating with antibacterial and anti-fungal washes and creams. Vets recommend wiping away discharge, clipping hair if necessary and lightly scrubbing with a warm medicated wash such as Troy Hoss Gloss. Leave for 10 minutes before rinsing and patting dry. Apply an antibiotic cream or ointment such as Filtabac with zinc, and repeat procedure daily for 2 to 3 days. Once the worst swelling has resolved, the cream can be replaced with a drying type of antibacterial spray such as Troy Chloromide.
Summer Mud Fever
WINTER mud fever causes problems by continual wetting of the limb (wet areas/mud) whereas SUMMER mud fever is instigated by ‘sunburn’ followed by fungal or bacterial infection. Summer mud fever is more common on legs with white socks and pink skin.
The ‘sunburn’ associated with summer mud fever is actually photosensitivity caused by ingestion of pasture or feed mycotoxins. Secondary fungal and bacterial infections then opportunistically invade the damaged skin barrier. Relying on the topical treatments that work for winter mud fever is not effective for treating summer mud fever whilst mycotoxins are active in the horse’s system.
Summer mudfever treatment requires use of adequate levels of broad-spectrum toxin binder along with antiseptic topical treatment and mineral supplementation. Removal from toxin infested pastures or use of an effective toxin binder usually results in skin clearing up relatively quickly (in a few days).
Sunburnt Noses
Some mycotoxins cause pink skin to become very sensitive to the UV rays in sunlight. Severe skin damage (which looks like really bad, blistered sunburn) can then occur even when horses have minimal exposure to sunlight.
Fortunately photosensitivity caused by mycotoxin ingestion is easy to combat – it’s simply a matter of adding a broad-spectrum mycotoxin binder as part of a diet containing balanced levels of copper and zinc as well as using a zinc-based sunscreen or Filtabac. Improvements will begin to be noticed within a few days provided the toxin binder targets the mycotoxins present and is fed at the necessary level of intake. In severe cases it may be necessary to remove the horse from the pasture or feed which is contaminated with mycotoxin.
Managing Horses with Skin Sensitivity
Vitamins and minerals play a very important role in skin health and immune function which impacts on the animal’s ability to cope with the inflammation, infection and immune challenge posed by mycotoxins, skin damage and irritation. Read here for tips on managing itchy horses.
Some species of grass are well known to favour mycotoxin-bearing fungi (e.g. ryegrass, paspalum) but most plants can harbour fungus at some point in their lives. Adding a broad-spectrum myctoxin binder to the feed daily or twice daily during humid weather and when ergot fungus is present on grass combined with applying a zinc-based sunscreen can yield very rapid and successful results in treating mycotoxin-caused photosensitivity and greasy heel symptoms.
Recommendations
Farmalogic recommends the following products for the treatment and management of horses with skin irritations relating to mycotoxins:
- A diet with correct mineral balance using the Equine Vit&Min best suited to your needs (365 days of the year) to ensure the body has all the nutrition it needs to function properly, repair itself and fight off immune challenges. This is one of the very important reasons that Farmalogic offers a free diet analysis service! Read here to learn the top 10 reasons why every horse needs minerals!
- A broad-spectrum toxin binder –choose one proven not to bind supplementary minerals. Farmalogic Grazaid contains the broadest acting toxin binder combination available in NZ and Australia which binds, traps and enzymically deactivates feed mycotoxins. Use when sypmtoms of mycotoxin ingestion occur or environmental conditions such as high humidity make mycotoxins prevalent. The amount of toxin binder needed depends on the amount of mycotoxin being ingested so it can take time to determine the required level of supplementation.
- Add antioxidants including natural vitamin E, organic selenium and SOD enzyme to deactive the free radical molecules that occur at sites of inflammation and injury. We recommend Farmalogic Melox for use during the treatment phase.
- Topical treatments for managing secondary infections, both fungal and bacterial. This can include washes or zinc creams but shouldn’t be ‘greasy’ or increase the moisture level of the damaged skin. We recommend:
- Troy Iodin – animal antiseptic which helps to prevent skin infections caused by bacteria and fungi (use during cleaning phase)
- Filtabac – antibacterial, zinc-rich wound protectant cream with sun filter properties (use during treatment phase)
- Troy Chloromide – an antiseptic insect and fly spray (use during final healing phase when a drying treatment is advised).
- Veterinary intervention with steroidals if required to bring inflammation under control to help the horse self-perpetuating the problem with rubbing or scratching.
Seek veterinary advice if symptoms persist.